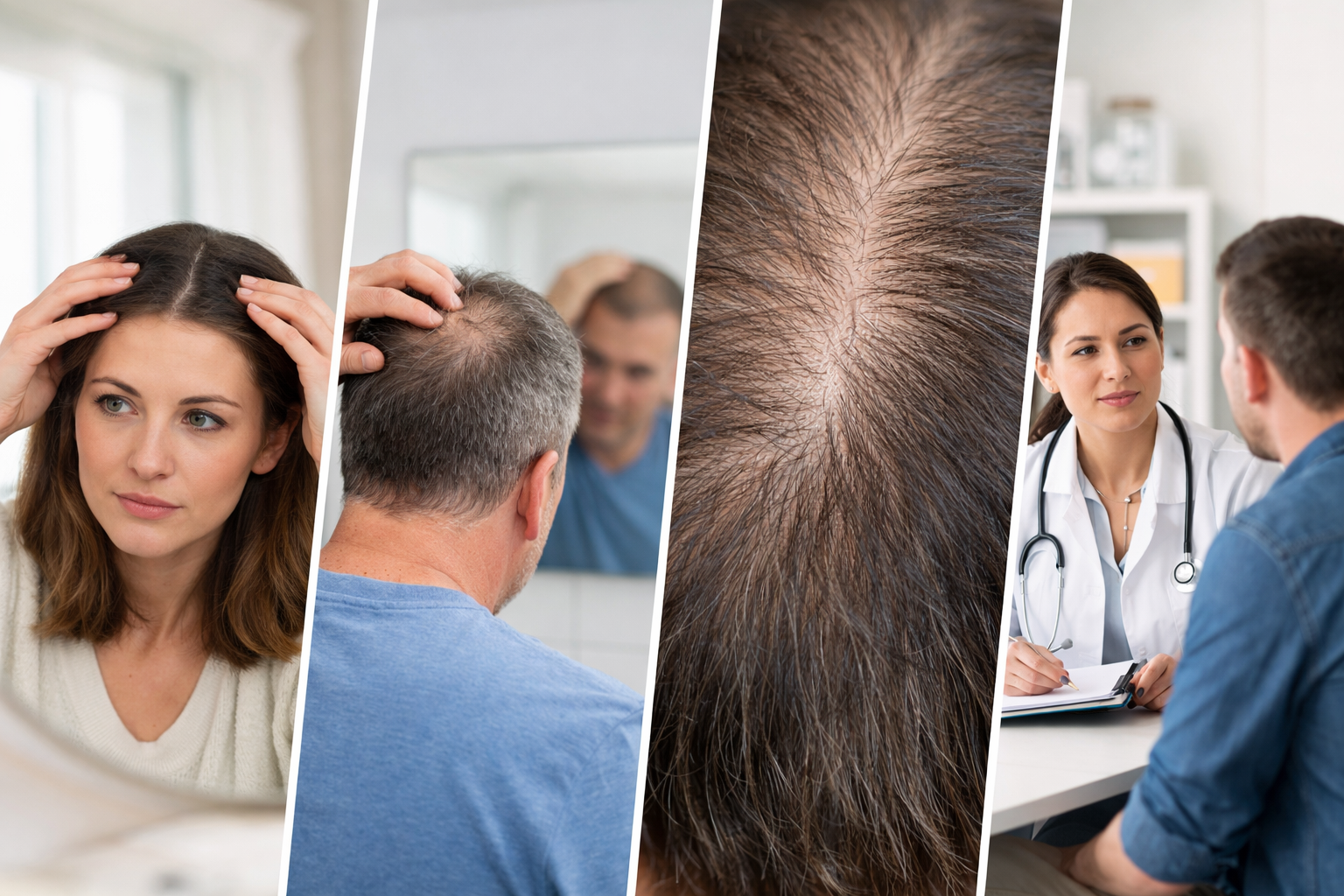
Testosterone for Women After Hysterectomy
The Missing Hormone No One Talks About
Many women who undergo a hysterectomy in their 30s are told:
“Your ovaries are still there. You won’t go into menopause.”
And technically, that’s true.
But what often isn’t discussed is this:
Even when the ovaries remain, ovarian hormone production frequently declines earlier than expected after hysterectomy, particularly testosterone.
And that decline can affect mood long before classic menopause symptoms appear.
Wait… Women Need Testosterone?
Yes.
Women produce testosterone from:
- The ovaries
- The adrenal glands
And testosterone plays a critical role in:
• Libido
• Motivation and drive
• Mood stability
• Lean muscle mass
• Bone strength
• Cognitive clarity
• Stress resilience
It is not a “male hormone.”
It is a human hormone.
What Happens After Hysterectomy?
Even if the ovaries are preserved:
- Ovarian blood flow may decrease
- Androgen production can decline
- Hormone signaling can shift
- SHBG levels may change
- Stress physiology often increases
Many women report subtle changes like:
“I don’t feel depressed… but I don’t feel like myself.”
“I’ve lost my spark.”
“I cry more easily.”
“I have no libido.”
“I’m exhausted but my labs are ‘normal.’”
These symptoms are often dismissed because estrogen levels may still appear adequate.
But testosterone is rarely evaluated.
Why Mood Changes First
Testosterone supports dopamine activity in the brain.
Dopamine influences:
• Motivation
• Pleasure response
• Focus
• Emotional resilience
• Initiative
When testosterone declines, women often experience:
- Emotional flattening
- Increased tearfulness
- Reduced stress tolerance
- Lower confidence
- Loss of ambition
It doesn’t always look like depression.
It often looks like diminished vitality.
The Under-Discussed Benefit: Mood Restoration
When testosterone is restored to physiologic female levels, many women describe:
“I feel steady again.”
“I can handle life better.”
“I’m not so emotionally fragile.”
“My confidence is back.”
It’s not euphoria.
It’s stability.
And for high-functioning women balancing careers, parenting, and stress, that stability matters.
Is Testosterone Safe for Women?
When used appropriately and monitored carefully, physiologic dosing can be safe.
Monitoring typically includes:
- Total Testosterone
- Free Testosterone
- SHBG
- Estradiol
- CBC
- Lipids
Dosing is conservative, far below male ranges, and individualized.
Potential side effects (dose dependent):
- Acne
- Oily skin
- Increased hair growth
- Voice changes (rare at proper dosing)
- Lipid changes if overdosed
This is why medical supervision matters.
Who Might Consider Evaluation?
Women who:
- Had a hysterectomy in their 30s or early 40s
- Feel emotionally flat without clear depression
- Have low libido
- Experience decreased motivation
- Struggle with strength loss or body composition changes
- Feel “not like themselves” despite normal labs
The Bigger Picture
Hormone health is not about chasing numbers.
It’s about restoring physiologic balance.
For some women, testosterone is the missing piece, especially after surgical changes to the reproductive system.
This conversation deserves more attention.
Because mood, vitality, and drive are not luxuries.
They are part of health.
If you’d like to learn more about hormone evaluation or schedule a consultation, contact Optimize by JaeNix to discuss whether testosterone therapy is appropriate for you.